 March 2024
March 2024
We are so proud of our founder, Steve Wagner for being recognized by The City of Phoenix for all his hard work!
Congratulations Steve Wagner!
He was chosen for the 2024 Community Service Award!
April 2023
Know the Difference: Cardiac Arrest vs. Heart Attack
Heart attack and cardiac arrest are two of the most common heart conditions. People often use both events interchangeably, but they are not the same. To understand their differences, it helps to know what happens in both processes. Here are some of the distinct characteristics of each condition, including symptoms and possible causes.
https://www.abrazohealth.com/healthy-living/corporate-content/know-the-difference-cardiac-arrest-vs-heart-attack/?
 February 2023
February 2023
New Arizona law requires lifesaving measures in assisted living facilities – KTAR [secure-web.cisco.com]
Steve Wagner is one of the thousands of Arizona firefighters who supported the bill. With 19 years on a firetruck, he has responded to several 911 calls connected to the issue this bill works to fix.
 February 2023
February 2023
Arizona Tax Credit
 January 2023
January 2023
We are so proud of our founder, Steve Wagner for being recognized by former Governor Doug Ducey for his hard work and dedication for helping to promote positive change for our most vulnerable population in Arizona! Well done!
 October 2022
October 2022
Father resuscitates 12-year-old daughter after she was struck by lightning in Sun City West
CPR matters! Per AZCentral.com, A father’s quick reaction and a little help from the Bee Gee’s, specifically “Staying Alive,” is what kept a 12-year-old girl breathing after she was struck by lightning. Her father performed CPR three times, once to the beat of the song, after she was struck by lightning during Saturday’s storms in Sun City West.
The girl, Ella, had stepped outside of her grandparent’s house to play with a friend when her father Steven Jorgensen heard loud thunder, saw a bright flash and saw her collapse.
Doctors say Jorgensen’s quick action is the reason his daughter is alive.
Jorgensen said he saw his daughter fall and immediately started performing CPR, which he learned while serving in the Marine Corps.
“I got her heart back going, I got her breathing, and it was only for a short amount of time until I lost her again,” Jorgensen said.
 September 2022
September 2022
a “silver tsunami”
(NEWSER) – American society is in the early stages of a “silver tsunami,” with adults over 65 expected to outnumber children by 2035. Demand for nursing homes will surge, as will revenues for those who operate such facilities, writes Yasmin Rafiei for the New Yorker. It’s an irresistible business opportunity for private equity groups and other for-profit companies, which collectively own about 70% of nursing homes. Many states have lax standards, and federal staffing requirements for such facilities are set at one registered nurse during the day and one licensed practical nurse in the evening, regardless of the number of residents. Rafiei’s take: Elderly Americans will likely suffer and die in the name of profit. She gives a real-world example.
For 147 years, the nuns at St. Joseph’s Home for the Aged in Richmond, Virginia, maintained a pristine facility imbued with warmth and love. It was one of 52 US homes run by the Little Sisters of the Poor, but they sold off many as the number of nuns in their ranks dropped. In June 2021, St. Joseph’s was bought by the private equity firm Portopiccolo Group, which now operates 130 homes. The home’s aquarium and aviary were pulled, and the quality of food sharply decreased. More concerningly, care allegedly declined, with Rafiei writing of “briefs so saturated with urine they’d turned brown” by the time they were changed in the morning. As Rafiei explains, staffing tends to be the top operating expense, so when private equity steps in, staffing is usually cut. Prior to the sale, the home managed to keep its COVID count to four infections and no deaths; in Portopiccolo’s first four months, there were 17 infections and 6 deaths. (Read the full story here.)
 September 2022
September 2022
Powers of Attorney: Crucial Documents for Caregiving
Get these important legal papers in place before you need them
by Amanda Singleton, AARP
What comes to mind when you hear the words “power of attorney”?
An important legal document? A license to steal? The key to successful caregiving? All of the above?
If you thought “all of the above,” you’re on the right track. The power of attorney is a powerful legal document.
It can give tremendous authority to another person, including the right to access your bank accounts and to make decisions for you. And, in times of crisis or declining health, a power of attorney is the essential tool in your caregiver’s toolkit.
Types of powers of attorney
A power of attorney names a person who can act on your behalf; this person is called your “agent” or “attorney-in-fact.” Before you create a power of attorney, you should know your options and which ones your home state allows.
Specific powers of attorney limit your agent to handling only certain tasks, like paying bills or selling a house, and generally on a temporary basis.
General powers of attorney give your agent broad authority. They can step into your shoes and handle all your legal and financial affairs.
With these documents, that authority can end at the time you become incapacitated.
Durable powers of attorney may be limited or give your agent broad authority to handle all your legal and financial affairs, but your agent keeps the authority even if you become physically or mentally incapacitated. This means that your family may not have to ask for a court to intervene if you have a medical crisis or have severe cognitive decline such as late-stage dementia.
Sometimes, medical decision-making is included in a durable power of attorney for health care. This may be addressed in a separate document that is solely for health care, like a health care surrogate designation.
Some states recognize “springing” durable powers of attorney, which means the agent can start using it only once you are incapacitated. Some states don’t, which means the day you sign the durable power of attorney, your agent can use the document.
The risks of not planning ahead
A well-drafted power of attorney helps your caregiver help you. It can keep the gears of your life turning if you cannot.
This means everything from applying for financial assistance or a public benefit such as Medicaid to making sure your utilities stay on and your taxes are paid. Trying to do any of those tasks without the proper document is almost impossible.
According to a 2020 Merrill Lynch report, 43 percent of Americans age 55 and older worry that they don’t have an advocate to look out for their interests as they age. Yet only a third of this age group has a durable power of attorney, the study found.
When I was my mom’s caregiver, I had to help her without a power of attorney for six months. She hadn’t created one before her diagnosis and was physically unable to see an attorney after.
It’s an understatement to say how stressful it was to get things accomplished and advocate for her without one.
Cancer took my mom’s voice, so she couldn’t vocalize her wishes in more than a hard-to-understand whisper. More times than I can count, I was asked to put her on the phone so she could authorize me to talk about insurance or an overdue bill.
It was so frustrating that I pretended to be my mom a few times, which is not legal or advisable. I also signed her hospital and facility admissions paperwork, which exposed me to being responsible for her bills.
We both feared that certain unpredictable relatives would try to take over her decision-making or possibly exploit her.
For those reasons and more, as soon as she was able, she had a durable power of attorney prepared. We both felt relieved and more secure from that day forward.
Prepare documents early, update frequently
Today, as a caregivers’ lawyer, I often hear from new clients who want me to prepare a power of attorney for their loved one with dementia.
Although a dementia diagnosis alone does not prevent a person from signing legal documents, we cannot ethically let a person sign if they are not “competent.” Basically, this means that they are not able to understand the implications of the document.
The only recourse if a person is not competent to sign legal documents may be a court procedure known as a guardianship or conservatorship. These can be expensive, time-consuming and contested by family members who don’t agree.
Assets can be depleted quickly, and relationships strained. The biggest risk as the care recipient is that you may not have a say in who will be the person the court appoints to make decisions for you.
So, please, don’t delay. All adults, from the age of 18, should have a power of attorney in place.
And if you have one, consider whether now is the time to update it. If you’ve moved states of residence, if you have property in multiple states like a vacation home or if you are a snowbird, if you live in a state that requires you to renew your power of attorney occasionally, or if your power of attorney is more than a few years old in any state, it’s well worth your time to speak with a qualified lawyer.
Your lawyer can also explain how to create your documents to limit possible exploitation and which additional documents complement your power of attorney.
With thoughtful planning and an understanding of your agent’s authority, a power of attorney will give you peace of mind that your wishes will be followed and your best interests protected in times of crisis.
Editor’s note: This article, originally published July 19, 2019, has been updated with more recent information and an AARP Top Tips video.
Amanda Singleton is a recipient of CareGiving.com’s national Caregiving Visionary Award and serves caregivers across their life span through her law practice. Follow her on Twitter and Facebook.
More Financial and Legal Help for Caregivers
 May 2022
May 2022
Auditor general hammers Arizona for falling short on nursing home complaint investigations
Arizona has put nursing home residents at risk by failing to properly investigate complaints of abuse and neglect in the facilities, a new auditor general’s report says.
Among the major problems identified in the report is a finding that the Arizona Department of Health Services inappropriately reclassified nearly all of its high-priority complaints and self reports about problems in nursing homes to lower priorities.
Changing the priority “artificially extended” the time frame for responding to the complaints from 10 days to a year, says the report, which based its finding on an analysis of 132 open complaints as of April 21, 2021.
The report, dated Monday, was completed by the independent Arizona Auditor General’s Office. It is a 30-month follow-up to a September 2019 report that faulted the state health department for the way it was investigating complaints about nursing homes and made five recommendations for improvement.
But none of the five recommendations from September 2019 were ever implemented, the latest report says. In addition, the latest report found “significant” failures with complaint prioritization and investigations “that have continued to put long-term care facility residents’ health, safety and welfare at risk.”
 January 2022
January 2022
Every minute counts after a stroke. Mobile scanners may be the breakthrough doctors need
It happens something like this. You’re talking with friends at dinner when your spouse asks why you’re slurring your speech. Or maybe you’re out for your morning walk when your movements suddenly turn jerky, as if half of the invisible strings that guide your limbs had suddenly been cut.
Maybe pain is the herald, a crushing migraine or a starburst in the back of the head. Maybe you’re alone. Or, worst of all, driving on the highway.
That’s how it was for Buddy Bailey, who at the time was a 70-year-old investment adviser, golf ball hunter and steadfast husband of 51 years. It was a bluebird day in Houston. Bailey was breezing south toward Galveston on a courtesy call to a valued client. The Gulf Freeway was just rising up to cross El Dorado Boulevard, and for a fleeting moment the view through the windshield was reduced to the gray race of the road and the untroubled sky.
There are no exact words for what happens next. Darkness, dizziness, the world withdrawing, inputs going dead. A silent, mindless, timeless drift through four lanes of traffic — and then being jolted awake by the crash of his Mercedes-Benz against the freeway barrier, and swerving back into the chaos and light. When the Benz finally comes to rest, Bailey knows the danger still hasn’t passed. Even so, there is nothing he can do. Because the violence is still taking place inside his head.
It is among the most feared medical emergencies. What else but a stroke could make you think you’d rather have a heart attack? Sure, heart attacks are more fatal, but at least if you survive you can carry on more or less as before — without a dimming of the mind or the loss of key bodily functions.
With strokes there is no such assurance. Fully 40 percent of stroke survivors require some kind of special care, 25 percent experience significant cognitive decline, and an average of 17 percent will be discharged into long-term care. This is not the vantage from which to sit back and reflect on one’s life accomplishments.
The comparison with heart attacks is not incidental. The vast majority of strokes — or “cerebrovascular accidents,” to use the textbook term — are caused by a blockage in blood flow. Yet unlike a heart attack, for which there are dozens of immediate interventions, a stroke has proven infuriatingly difficult to treat. More than 1,000 drugs have been tested—mostly to no avail. The lack of progress has led researchers to explore offbeat solutions. Brain cooling, transcranial magnetic stimulation, lasers delivered through the nose. Drugs derived from peach pits and the venom of the Malayan pit viper. By the early ‘90s, doctors were no closer to finding a treatment for strokes than they had been 50 years prior. It was “diagnose and adios,” as the saying went. Nothing to be done.
Stroke is a story of anguish and frustration. Although the Food and Drug Administration (FDA) has approved two treatments (a medicine, tPA, that can break up the clot in a minority of strokes and, in 2016, a surgical procedure to remove clots from a sufficiently large blood vessel), people are still dying by the thousands — 150,005 in 2019. This has led some people to look for other solutions. And in the past several years, a new approach to strokes has been gaining adherents all over the country. One day it might save your life.
The mobile stroke unit (MSU) is a specialized ambulance equipped with a portable CT scanner. Rather than take stroke patients to a hospital, the idea is to take the hospital to the patients. The onboard scanner allows the doctor to diagnose en route to the hospital, eliminating the transport time, which could be as much as 40 minutes.
With a stroke, those minutes matter. Currently, only 1.3 percent of eligible patients receive treatment in the first hour after having a stroke, and nearly 20 percent are treated between three and 4 and a half hours later.
Brain tissue dies fast. For every 30-minute delay the relative likelihood of surviving a stroke with no deficits decreases by 15 percent. By eliminating some of those minutes, MSUs could (in theory, anyway) save millions of brain cells — and perhaps thousands of lives.
The key is the CT scanner, a doughnut-shaped X-ray machine capable of rendering 3D images of the brain. The scanner determines the kind of stroke the patient is having — hemorrhagic or ischemic. An ischemic stroke is caused by a blood clot that cuts off blood flow to the brain. A hemorrhagic stroke — seven times less common but four times more deadly — is caused by an aneurysm or burst blood vessel. The difference matters, because tPA, the only drug available to treat strokes, works only for ischemic strokes. When given for a hemorrhagic stroke, it can be fatal.
The MSU serves an important role here, triaging patients so they can be quickly routed to the most appropriate care. Bailey’s clot, for instance, was a big one. This made it more dangerous. But it also made him a candidate for a thrombectomy which, combined with an early tPA intervention, gave him a far greater chance for reduced disability — and an 11 percent greater chance of returning to the same level of health he had before the stroke. Ordinarily, less than 3 percent of patients receive tPA within the golden hour. With the MSU, Grotta raised that number to 33 percent. As a result, these people, Bailey among them, survived their strokes with minimal or no disability — 10 percent more than the non-MSU group.
Why wait around for the problem to come to you, when with the right set of wheels you can go to the problem?
 September 1, 2021
September 1, 2021
National Preparedness Month
National Preparedness Month (NPM) is an observance each September to raise awareness about the importance of preparing for disasters and emergencies that could happen at any time.
National Preparedness month begins this week with a focus on making sure you are prepared for an emergency at home, work or places you visit.
*Talk to your friends and family about how you will communicate before, during, and after a disaster. Make sure to update your plan based on the Centers for Disease Control recommendations due to the Coronavirus.
*Gather supplies that will last for several days after a disaster for everyone living in your home. Don’t forget to consider the unique needs each person or pet may have in case you have to evacuate quickly. Update your kits and supplies based on recommendations by the Centers for Disease Control.
*Natural disasters don’t wait for a convenient time. Preparing for them shouldn’t wait either. Start today by signing up for alerts, safe-guarding important documents, and taking other low cost and no cost preparedness actions to lessen the impact of disasters and emergencies for you and your family.
*Talk to your kids about preparing for emergencies and what to do in case you are separated. Reassure them by providing information about how they can get involved.
 August 15, 2021
August 15, 2021
Nine Heart Attack Symptoms
There are nine symptoms that could signal you are having a heart attack. If you begin to experience these symptoms, seek help immediately. Put your health first. Don’t ignore the signs, they could save your life. Not all people who have heart attacks experience the same symptoms or to the same degree.
- Chest pain or discomfort
- Chest pain that comes and goes and returns
- Pain in shoulder, arm, back, neck, jaw or stomach
- Lightheadedness or fainting
- Sweating
- Fatigue
- Shortness of breath
- Nausea or vomiting
- Pain in back or jaw
If you think you are having a heart attack, call 9-1-1 immediately for an ambulance to take you to the hospital. Do not try to drive yourself.


June 14, 2021
Immediate resuscitation saves lives! Amazing story of survival.
The Euro 2020 match between Denmark and Finland resumed Saturday nearly two hours after Danish soccer player Christian Eriksen collapsed in the first half of the game.
The star midfielder was walking alone near the sideline around the 42nd minute when he appeared to stumble and then fall forward. His teammates urged trainers to rush to his aid.
Eriksen’s teammates then formed a ring around him as medics performed CPR.
Players from both teams were in tears, as the stadium in Copenhagen, Denmark, fell silent, NBC Sports reported.
“Please God,” Fabrice Muamba, the former Bolton Wanderers midfielder who collapsed after suffering a cardiac arrest during a televised FA Cup game in 2012, wrote in a tweet.
Eriksen is awake, according to Denmark’s soccer governing body. However, further examinations will be conducted, officials said.
The game was suspended due to the medical emergency, but UEFA “agreed to restart the match” after receiving requests from players of both teams.
“At these times, the unity of the football family is so strong and he and his family carry with them the good wishes and prayers of everyone. I heard of fans of both teams chanting his name. Football is beautiful and Christian plays it beautifully,” he added.
 May 16, 2021
May 16, 2021
Ducey closes nursing home board after disaster at Granite Creek center
Arizona’s nursing home board approved a felon to run a Granite Creek home and 15 people died. Now, Gov. Doug Ducey is terminating the board.

May 6, 2021

April 8, 2021
National Healthcare Decisions Day – April 16
National Healthcare Decisions Day (NHDD) held April 16 each year, was created to inspire, educate and empower the public and providers about the importance of advance care planning. Having these thought-provoking conversations—and then documenting them for healthcare providers to access in real-time—ensures your wishes are honored in almost every possible medical situation.
April 1, 2021
Learn about The RightCare Foundation and SB1373
 March 16, 2021
March 16, 2021
Vaccine Shines A Light on Dark Days on Nursing Homes
With Covid-19 cases dropping by 83% within 2 months in nursing home staff, this is promising news for the residents. The Centers for Medicare and Medicaid (CMS) and Centers for Disease Control (CDC) issued updated guidelines for nursing homes and allowing more visitation. The guidelines allow indoor visitation at all for all residents, regardless of the vaccination status of the resident or their visitor(s). The guidelines also expand the boundaries of “compassionate care” visits, regardless of vaccination status. Compassionate care visits entail visitations to a resident whose health has experienced a significant change or decline.
While there are limitations regarding unvaccinated individuals, this is ecstatic news for the residents who have gone an extended period of time without seeing their loved ones. Evan Shulman, the director of CMS nursing homes division, tells USA Today that he has heard residents state that they would “rather die of COVID-19 than go any longer without seeing family”. Many family members worry about the quality of care their loved ones are receiving behind closed doors. Because the pandemic has taken a great toll on the residents for both their mental and physical health, the visitation expansion could be a breath of fresh air. The rise of vaccination rates within the nursing home staff could also reduce the likelihood of residents contracting COVID-19.
535,000 people have lost their lives to COVID-19, according to the New York Times. There has been about a 26% decrease in cases and a 53% decrease in coronavirus deaths over the last 2 weeks in the state of Arizona. While there have been 2.66M doses administered to individuals within Arizona, over 85% of the population is not fully vaccinated. Many nursing homes have not mandated the vaccine due to fear of losing employees and liability concerns.
Despite the controversial opinions regarding the COVID-19 vaccine, it has returned a plethora of our “normal” activities back. Although there has been a lift of pandemic restriction orders which could increase the likelihood of spreading the virus, being fully vaccinated can help protect the public against illness through herd immunity. The public can only remain hopeful that our lives will go back to “normal” and the vaccine helps eliminate the COVID-19 virus.
https://www.cms.gov/files/document/qso-20-39-nh.pdf
https://www.nytimes.com/interactive/2020/us/coronavirus-us-cases.html
https://github.com/owid/covid-19-data/blob/master/public/data/vaccinations/us_state_vaccinations.csv
 March 1, 2021
March 1, 2021
Right place at the right time
The celebrity doctor had just returned from a Florida trip when he needed to spring into action.
Famed medical expert Dr. Mehmet Oz was in the right place at the right time on Monday night when a man at Newark Liberty International Airport was in urgent need of emergency medical assistance.
“Last night, a man collapsed near me and my family after we arrived at Newark Airport,” he told Travel + Leisure on Tuesday. “I performed CPR with the help of a Newark Port Authority police officer and cleared the man’s airway. Thankfully, Newark Airport had a defibrillator nearby that we were able to use to save his life.”
The surgeon, and host of The Dr. Oz Show, was with his wife and daughter, having just returned from Palm Beach, Fla. when the incident occurred. He worked alongside the Port Authority officers, who also thanked him and the officers on duty for their heroic efforts on social media- “Thank you @DrOz and our brave PAPD team of officers Michael Bock, Matthew Vecchione, Daniel Olbrich, and Jeffrey Croissant who provided life-saving #CPR to a passenger in cardiac arrest last night at @EWRairport,” the PAPD account tweeted.
A photo of Oz and the officers responding to the scene was shared on Twitter by a supposed fellow passenger.
“As a physician and a human being, it’s our responsibility to jump in when there’s a medical emergency,” Oz told T+L. “[This is] another critical reminder of how important it is to take the time to learn how to do CPR and use a defibrillator. You could save a life.”
We’re told Oz has been keeping in touch with the man’s wife by text message and phone. The man is still in the hospital undergoing testing.
February 16, 2021
Arizona bill aims to require lifesaving care in assisted living facilities
Share
BY ALI VETNAR | FEBRUARY 16, 2021 AT 4:45 AM
UPDATED: FEBRUARY 16, 2021 AT 8:48 AM
PHOENIX – A new Arizona bill looks to obligate caregivers in the state to perform lifesaving measures if a patient experiences a medical emergency while inside an assisted living facility.
Introduced by Republican State Rep. Nancy Barto, SB 1373 would require assisted living facilities and their employees to have an affirmative duty of care for their residents.
That includes basic life support, initiating immediate cardiac resuscitation before firefighters or other emergency medical services arrive – in accordance with the resident’s advance directives and do-not-resuscitate order.
While many of the near 3,000 assisted living facilities in the state market themselves as medical care providers, it’s believed some choose not to. How can that be? The law doesn’t require it.
Although caregivers in Arizona are required to be CPR certified and first-aid trained, the law does not mandate them to use it.
This bill comes after frustration and skepticism has grown over many assisted living facilities in Arizona choosing not to perform the lifesaving care and instead relying on first responders for solutions.
Steve Wagner is one of the many Arizona firefighters who respond to the 911 calls connected to this issue.
“Sometimes we are really frustrated when we arrive on the scene and we see, we know what the results are going to be based on what was or what was not done prior to our arrival,” he told KTAR News 92.3 FM on Friday.
As a paramedic firefighter, Wagner described his frustration talking about the importance of CPR.
“The brain can survive for up to about six minutes after the heart stops. If CPR is started within six minutes of cardiac arrest, the brain may survive the lack of oxygen. After about six minutes without it [CPR], however, the brain begins to die,” Wagner added.
Wagner has experienced this same issue time and time again in his 19 years on a fire truck. That’s why he created the RightCare Foundation.
The nonprofit teaches the best practices in response to cardiac arrest and advocates for time-critical pre-EMS care and community engagement to better equip organizations and individuals.
Although caregivers want to do the right thing – why is this care not being administered in the first place within some of the state’s assisted living facilities?
“It comes down to the folks that pay attention to liability, like all the lawyers – essentially saying, well in Arizona there is no affirmative duty to use the training – so don’t,” Wagner described.
According to the AZleg.gov, the bill is supported by AARP, multiple cities in Arizona and the Professional Fire Fighters of Arizona.
Arizona Assisted Living Federation of America, the AZ Health Care Association and the Arizona Assisted Living Homes Association are among those who oppose SB 1373 and the duty of care.
The progress of the bill can be followed online.
February 1, 2021
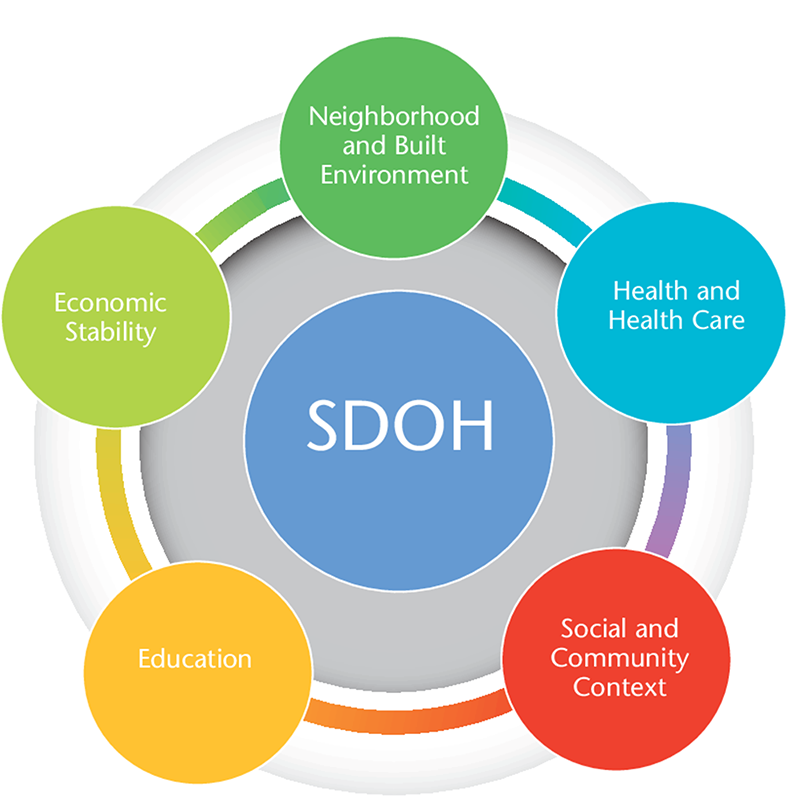
Covid-19 Vaccine and the Impact of Social Determinants of Health
With over 11 million cases of Covid-19 and 245 thousand deaths in the United States alone, there is a strong demand for a vaccine. The Covid-19 pandemic has impacted the entire world and taken many lives. Families and friends are unable to see each other. People in nursing homes can only talk to people through a window. Many are dying in hospitals on an incubator all alone.
There are multiple potential vaccines in development. However, it is uncertain when a vaccine will be available to the public. Vaccines help to train the immune system how to combat a disease. Vaccines can also allow for herd immunity. Herd immunity is when the majority of the population is vaccinated and those who are unable to receive a vaccination are still protected. However, it requires for 90% or more of the population to be vaccinated depending on the disease.
When a Covid-19 vaccine is released, it will not immediately be readily available to the public. There is simply too high of a demand. Because of this, the National Academy of Medicine states in its report that individuals who are socially vulnerable to Covid-19 should be the ones to receive the first vaccinations. A summary of the report can be found here. The social vulnerability of a population is measured through the Centers for Disease Control and Prevention’s (CDC) Social Vulnerability Index. This index identifies different social determinants of health (SDoH).
According to the Center for Disease Control and Prevention (CDC), the people who are most at risk for Covid-19 are the elderly and people with medical conditions. However, your
individual situation can also determine how at risk you are. This is known as social determinants of health.
Social determinants of health include economic status, education, social support, access to healthcare, and more. SDoH impacts the chances of becoming infected and dying of Covid-19. For example, those who live in rural communities, those who are homeless or refugees, people living in nursing homes, and assisted living are all more susceptible to dying from Covid-19. Other things like race and ethnicity also have an impact. HealthyPeople 2020 wants to address the importance of social determinants of health and its impact. They wish to take action on SDoH and create a world with more health equity so that everyone is able to receive optimal care no matter their background.
It is important to address social determinants of health in families and in communities to better understand what can be done to improve the health of the population. Those who are very socially vulnerable whether it is because they are poor and have very little access to care, or because they are old and living in an assisted living facility are going to be more defenseless against any virus or disease.
The people who are most at risk of dying from Covid-19 will most likely receive the vaccine first. Next will be those who are likely to encounter people who have Covid-19 such as healthcare workers and first responders. Since the vaccine will not be mass produced right away, those who have proven to be more susceptible to Covid-19 the best way to decrease the death rate from Covid-19 would be to give the vaccination to those who are most vulnerable first.
This is the first time the first time in history where a specific population is prioritized in receiving a vaccine. Covid-19 is mostly impacting the elderly and those with preexisting health conditions; however, it is also disproportionately affecting people of color. Families and communities with a low socioeconomic status are also more likely to be impacted by a virus. Other social determinants of health are having a major impact on who is being impacted by Covid-19.
The RightCare Foundation believes in health equity and positive health outcomes. We want to help to improve peoples’ lives and have everyone receive the care they want and deserve. Our goal is to provide best practice care. We value all lives no matter someone’s background or their wealth.
 December 29, 2020
December 29, 2020
As we close out the year 2020 and reflect back on what is important in life, we look forward to a better year ahead. Together with your help we can promote change. Please join us in the fight for best practice care for all. Your contribution will help advance programs and policy change to help secure that everyone has the care and respect that they deserve. Thank you for your support!
 December1, 2020
December1, 2020
The Growing Problem of Elderly Abuse in the United States
Those who are living in assisted living facilities or nursing homes are at high risk of abuse. This is because many of them have limitations in both their mental and physical health. Many people in nursing homes have gone into them because they are no longer able to care for themselves and are in need of daily medical assistance. For those who are suffering from mental illnesses it can be very difficult for them to communicate with others when they are being abused or when they are not being given the care they need.
When there is an incident of abuse in a nursing home, the staff and medical professionals must report the abuse incident within 48 hours. Failure to do so can result in fines, criminal action, or even closing of the nursing home. This is a state and federal law.
There are many forms of abuse. Some forms of abuse include physical, mental, financial, abuse, neglect, and even social isolation. According to Nursing Home Abuse Statistics, as many as 1 in 10 people over the age of 60 have experienced some type of abuse. It is also believed that only 1 in 14 incidents of elder abuse are reported, while another study suggests that only 1 in 25 abuse cases are reported.
According to the adult protective services annual report SFY 2018, there were 4,257 investigated abuse allegations, 3,256 neglect allegations, and 3,748 exploitation allegations in Arizona in the year 2018 alone. Not every report is investigated, not everyone who experiences abuse files a complaint. Special focus facilities are nursing homes that have received low inspection scores by the Center for Medicaid and Medicare and are put on a national watch list. You can find a list of facilities in Arizona that have made the special focus facilities here.
One survey of 577 nursing home staff, found that 36% had witnessed at least one incident of physical abuse and 81% reported that had observed and 40% had committed at least one form of psychological abuse within a 12-month period. However, very few of these incidents were ever reported and the nursing homes were not fined or shut down.
A new study from CBC marketplace analyzed 632 nursing homes in Ontario, California and found that 85% were repeat offenders of violation codes. It also showed that 101 homes have repeatedly failed to report abuse that had occurred. The family of one woman who was physically abused wants there to be consequences for the facility where the abuse occurred, however it seems unlikely to happen.
Nursing homes and assisted living facilities are not being held accountable for abuse. Those who are in assisted living facilities are unlikely to report abuse because they are unable to.
More needs to be done to help prevent different types of abuse in nursing homes and healthcare providers need to begin holding each other accountable and report elderly abuse. This can help improve the quality and longevity of life for people in nursing homes and assisted living.
Here at RightCare our goal is to ensure that people are treated with the care they deserve and to hold those accountable who are not providing adequate care. We want a world where people can put their trust in nursing homes and assisted living facilities. Nursing homes and assisted living facilities need to report instances of abuse and there needs to be more staff training on elderly abuse as well as how to report it.
If you or a loved one has a story of abuse or neglect in a nursing home or assisted living facility and would like to share it, please contact us at enter email us at infor@rightcare.org to help the RightCare foundation change policies in nursing homes.
 November 14, 2020
November 14, 2020
Innovative solutions being done in nursing homes to help combat isolation and loneliness.
Nursing homes have been hit badly due to Coivd-19. People over the age of 65 with preexisting medical conditions are the most at risk. Around 1/3 of adults over the age of 65 have a preexisting condition. Because of this, it is extremely important to keep those in nursing homes and assisted living facilities safe and socially distant. However, an increase in loneliness and depression in nursing homes because of not being able to see loved ones has occurred.
Before the pandemic, around 43% of adults in the United States aged 60 or older reported feelings of loneliness or isolation. Now with the pandemic limiting the elderly from seeing their family, there are sure to be more cases. Consequences of loneliness can include increased risk of heart disease, depression, dementia, and in severe cases, death.
Meals and activities in nursing homes that were once done in groups are now done alone. If someone wants to see their family, it must be scheduled in advance and through a glass window. People in nursing homes are no longer able to hold their family members for fear of getting the virus.
However, many facilities are doing their best to ensure that patients do not loose hope. They are creating hallway bingo, karaoke, and other fun activities that residents can participate in but stay socially distant.
AARP is helping connect people through a service called Friendly Voice. Friendly voice was created during the Coivd-19 pandemic to help combat loneliness. It is a program consisting of trained volunteers who call and check on folks from 9-5 on Monday-Friday. It offers hope to those who are isolated. Giving people someone to talk to can help to improve their mood significantly.
One nursing home helped to set up a beautiful wedding so that the mother of the bride would be able to attend. Originally, they were just going to have the wedding in the parking lot after their large wedding had to be cancelled due to Covid-19. However, the staff at Park Vista nursing home helped to set up a social distant area in their courtyard. Masks were handed out and everyone sat six feet apart. This enabled the bride to still have a beautiful and safe wedding that her mother was able to attend. The nursing home staffed helped to create a memory that the bride or her mother will not forget.
When nursing homes take the time to provide activities for their residents, they feel more involved and are less likely to feel lonely and isolated from everyone. Happiness can help benefit one’s entire body. People who are joyful are less likely to have a heart attack and more likely to have lower blood pressure, cholesterol, and stress levels.
RightCare is all about helping others and saving lives. We want to make sure that people have quality end of life care and are treated with respect. We also want to ensure the safety of people in nursing homes and assisted living facilities as well as end of life wishes.
 October 30, 2020
October 30, 2020
One in four Arizona nursing homes didn’t meet basic infection controls
In Arizona, for a private room in a nursing home the average monthly cost is $7,908 or just under $100,000 each year. However, many nursing homes still do not have proper equipment to prevent against the spread of Covid-19, while others are not taking proper precautions. People are paying thousands of dollars, yet nursing homes are not safe for them in the fight against Covid-19.
One of nursing homes’ main goals should be in the prevention of infectious diseases. This is because most people in nursing homes are over the age of 65 and may have multiple underlying health conditions. The prevention of the spread of a disease can save lives. However, one in four nursing homes in the state of Arizona have not been following procedures to help prevent the spread of Covid-19. Those who are living in nursing homes are at very high risk of dying from nursing homes, yet their care givers are not aiding in their protection against Covid-19. Nursing homes were cited for not properly wearing masks, sanitizing their hands, failing to keep residents socially distant, and other things that were aiding in the spread of Covid-19 as well as other diseases. 43 nursing homes were recently cited for these errors, half of whom had previously made mistakes in disease prevention.
Nursing homes continue to have a large number of cases of Coivd-19 as well as a large percentage of the deaths from Covid-19. This number may be higher since some nursing homes have refused to share the number of cases they have had until March. This is when Doug Ducey released an executive order stating that nursing homes need to report the number of new cases they have as well as the amount of personal protective equipment.
Meaning all of the positive cases from before March 11, do not have to be shared. Since a large number of positive cases in a nursing home would create a negative image for the facility, many choose to only report the ones after March 11.
People living in nursing homes are an at-risk population, however, the precautions that need to be made in order to prevent more deaths are not being made.
Here at RightCare we want to ensure that people living in nursing homes and assisted living are being protected and given the best possible care. We want a world that is held accountable for their actions. Nursing homes need to do better in order to protect the lives of their residents as well ensure they are receiving proper care.

October 15, 2020
Nearly 1,000 people each day in America experience cardiac arrest. The majority of people who experience cardiac arrest outside of the hospital will not receive the immediate care that they need. Only 6% of people who experience cardiac arrest outside of a hospital will survive, the majority of them will die before even reaching a hospital.
When someone is experiencing cardiac arrest, the sooner they receive proper chest compressions, the more likely they are to survive. The first few minutes that a person is experiencing cardiac arrest are the most crucial, however many people do not receive proper aid that could significantly improve their chances of living. According to the CDC, it is important to increase awareness about early prevention, using an AED, and performing compression only CPR. This can help reduce mortality and morbidity rates.
According to Cleveland Clinic Heart Health Survey, only 51% of Americans claim to know how to perform CPR. However, only around 16% know that they should only do chest compressions on adults unless it is the case of drowning or drug overdose. Even then, only 11% of Americans know the speed to give chest compressions. However, when someone is there to give chest compressions, their chances of survival increase significantly. When someone is given care immediately from a bystander when they experience cardiac arrest, they have a survival rate of 45%. This is because those first few minutes to receive help are crucial. When one is not administered help right away, oxygen is not being delivered to the brain and each minute that passes, the chances of death begin to increase greatly. Even if someone were to survive after not being receiving care for more than a minute, the chances of them having permanent brain damage is high.
It is important to teach people how to give CPR, but also how to give someone CPR correctly and only give chest compressions. According to the American Heart Association, “once chest compressions are begun, it takes time to develop cerebral and coronary perfusion pressures. When chest compression is interrupted for rescue breathing, the cerebral perfusion pressure drops abruptly, and the cardiac perfusion pressure drops significantly.” This means that when someone stops performing chest compressions to give two breaths, blood and oxygen is no longer being pumped to the brain which can cause significant damage. If more people knew how to give chest compression only CPR and how to do it correctly, a lot of lives would be saved in the United States. Arizona has begun to push for better outcomes and for people to have give chest compression only CPR. Dr. Gordon Ewy, a cardiologist in Tucson, AZ, helped realize the importance of chest compression only CPR, and Ben Bobrow, MD, helped convince emergency some emergency responders in the state of Arizona to adopt Cardio-Cerebral Resuscitation. This provides continues chest compressions and helps to increase survival rates significantly.
With correct training, lives can be saved, and outcomes can improve significantly. One major place that cardiac arrests happen outside of the hospital is in nursing homes and assisted living facilities since they have a high percentage of elderly people. However, many nursing homes, even in the state of Arizona, have a policy to only call the ambulance. Instead of helping in ones most desperate time of need they stand by.
Here at RightCare we seek to change this. We believe that everyone has a right to the best care. We want to help properly train people how to give CPR in order to save a life. We also believe that people should be held accountable for helping others, especially those who are in need of life-saving support.
 October 2, 2020
October 2, 2020
Can You Prevent Sudden Cardiac Arrest?The word “sudden” may sound inevitable. However, depending on your risk factors – and even if you seem healthy enough – there are steps you can take to lower your risk of sudden cardiac arrest. Spend a few minutes to prepare now and prevent surprises later. |
| See Heart Helpers |
 September 30, 2020
September 30, 2020
Healthcare Facility owes Arizona nearly 12 million dollars, former executives indicted for fraud
According to the Arizona Attorney General, Hacienda Healthcare’s former executives are being indicted for fraud. The Division of Developmental Disabilities (DDD) had a contract with Hacienda that paid $1,100 per patient, per day. If Hacienda was to receive an overpayment, they were to reimburse the (DDD). The chief executive officer, William Timmons, and the chief financial officer, Joseph O’Malley, are both being charged with fraudulent schemes and artifices as well as illegally conducting an enterprise. They misallocated funds from the DDD by manipulating costs to avoid repayments of state funds. This was done by inflating salaries and bonuses. Timmons and O’Malley also used the money to pay for a large sum of costs at Hacienda’s other facilities without any reimbursement. They ended up getting millions of dollars of overpayment by the state. “This settlement provides a pathway for Arizona to recover funds misused for years by Hacienda,” says Attorney General Mark Brnovich.
Hacienda is a healthcare facility and a certified nonprofit. It is supposed to do good, yet it stole millions of dollars from Arizona taxpayers and still did not give quality care to its patients. The same healthcare facility was in the news after a family’s daughter was raped and impregnated by one of the staff members. “She was in a vegetative state on a ventilator with no way to communicate.” According to the lawsuit she “was repeatedly sexually assaulted.” The other healthcare employees there claim they had no idea she was pregnant. It was looked into after a 911 call from the facility and it is believed that she was sexually abused on many accounts.
Many people who are in assisted living facilities cannot speak for themselves which leaves them vulnerable to being easily taken advantage of. The same goes for nursing homes. The people living in these facilities are prone to having mental disabilities as well as health issues. The RightCare Foundation’s goal is to save lives and promote best practice care. We strive for change so that people can receive great care and still have their end of life wishes honored. We strive for a world that is responsible and accountable to ensure that caregivers are providing excellent care.

September 25, 2020
Isolation due to pandemic has resulted in thousands of deaths from nursing homes.
It is important to practice social distancing, especially among the elderly and those who are at a greater risk from dying due to Covid-19. However, 1.4 million people in the United States are living in nursing homes and losing the hope that they will ever see their family again. There have been over 13,000 more deaths due to dementia in the United States since March than previous years.
Nursing homes continue to have insufficient testing, funds, and equipment against Covid-19. The Coronavirus Aid, Relief and economic Security (CARES) Act, provided $2.07 trillion to help American people from the health and economic impacts of Covid-19. Yet only 5 billion or .2415% of it is going to nursing homes. Almost 40% of Covid-19 deaths have been related to nursing homes. It is as though the United States doesn’t care about our elderly population.
Those living in nursing homes live very close together. The average age of people in a nursing home is 79. People who are aged 65 and older are at a higher risk of dying from Covid-19. Those who have underlying health conditions are also more prone to require hospitalization or to die from Covid-19. Nursing homes are filled with an elderly population who often have multiple underlying conditions, yet little is being done to protect them. Many nursing home residents do not have enough masks to go around. According to the Covid-19 Daily Report, as of June 30, 2020, Maricopa county residents who resided in nursing home or a long term care facility accounted for 19% of the deaths in Maricopa due to Coivd-19 and 25% of the hospitalizations, although this number is believed to be higher.
The loved ones of people in nursing homes are often strong advocates for their family member to receive proper care. Loved ones often inform staff of a certain food residents may or may not like. They may also ensure that they are eating all their food and staying hydrated. The nursing home staff does not have time to spend hours with each patient to learn and observe these differences. Many nursing homes are still not opening their doors to families in hope of protecting the patients’ health. Although it may help protect residents there from Covid-19, it is causing severe mental illnesses.
Though many nursing home residents are not receiving the care and visitation they deserve, it is important to keep a positive attitude. Positive thinking can help to improve health and longevity. Unfortunately, it is becoming very difficult for those in nursing homes to have a positive attitude and many are losing hope. There has been an increase in depression and feelings of loneliness since the pandemic has started causing nursing homes to shut down. This is leading to more deaths and increased mental decline among the elderly. Main symptoms of depression are difficulty concentrating and mental decline increases rapidly sometimes becoming impossible to reverse.
Read more on this at https://www.washingtonpost.com/health/2020/09/16/coronavirus-dementia-alzheimers-deaths/?arc404=true
RightCare advocates for proper training of nursing home staff, better equipment, and improved overall care for patients.
 July 29, 2020
July 29, 2020
Are you ready and willing to save a life? RightCare believes that your survival should not depend upon your Zip code
David Schlinkert, policy analyst, Morrison Institute for Public Policy
Melissa Kovacs, Ph.D., associate director of research, Morrison Institute for Public Policy
Policy Brief Excerpt:
When it comes time to check a mother, father or grandparent into a senior care facility, families want to know that staff will make every effort to respect both their loved ones’ health and wishes.
First responders called to a senior care facility for a cardiac arrest emergency want no less, with their duty focused on saving a life but also respecting a loved one’s wishes.
According to some firefighters in Arizona, two things often get in the way of that goal:
- Staff at senior care facilities fail to begin resuscitation before first responders arrive, making lifesaving opportunities all the more difficult with every passing minute.
- End-of-life wishes, called Advanced Directives, are not readily available to first responders, essentially tying their hands on what course to take.
First responders in such situations are forced to either:
- Save seniors in their twilight days who might not want to be saved; or
- Resuscitate seniors who want to be saved, but due to confusion and delay by facility staff, highly likely will suffer brain damage if saved.
It takes Arizona firefighters approximately 8 minutes to arrive at a senior care facility.
Brain damage begins after 5 minutes without oxygen.
 June 20, 2020
June 20, 2020
Our newest manikin technology has live and summative QCPR performance feedback, multiple student monitoring, and a gaming element to increase engagement are all available from the palm of your hand with the free QCPR Instructor and QCPR Learner apps. QCPR Technology is utilized to enable both instructors and trainees to more effectively monitor and review CPR performance, increasing the efficiency and value of training time.
 May 28th, 2019
May 28th, 2019
Our Senate Bill 1352 passed and is waiting for Governor Ducey to sign! Thanks to everyone who helped keep this Bill moving. With this Law, we will keep saving lives and honoring wishes in Arizona!
Read SB 1352 – Introduced by Senator Carter
RightCare Foundation, The AZ Hospital and Healthcare Assoc. and many other organizations were in support of SB1352. It is legislation that will improve effectiveness of health care directives Arizonans can use to ensure their healthcare wishes are honored at the end of life. This bill will make Healthcare Directives in the state registry accessible to EMS and all healthcare providers.
Facts About Senate Bill 1352 Health Care Directives Registry; Transfer
What’s the problem?
In 2004, the legislature created a framework for a statewide health care directive registry. The current system, however, limits medical providers’ efficient access to the registry and hinders providers’ ability to follow an individual’s directions for their health care.
What’s the solution?
SB 1352 improves the effectiveness of the Arizona Health Care Directives Registry by transferring it from the Secretary of State to a Qualifying Health Information Exchange that is approved by the Arizona Department of Health Services.
Does this really affect me?
Health Care Directives are legal documents that capture a person’s wishes regarding medical treatment or identify an individual who has the legal authority to make medical decisions on a person’s behalf.
Who supports SB1352?
Lots of people including legislators. All 30 Senators voted for it in the Senate and all nine committee members voted from it in the House Health & Human Services Committee. Additionally, the following organizations support it:
AARP ● Alzheimer’s Association Desert Southwest Chapter ● Arizona Ambulance Association ● Arizona Alliance For Community Health Centers ● Arizona Association of Health Plans ● AZ Chapter American College of Emergency Physicians ● AZ Council Of Human Service Providers ● Arizona Health Care Association ● Arizona Hospital and Healthcare Association ● Arizona Medical Association ● Arizona Nurses Association ● Arizona Osteopathic Medical Association ● Banner Health Arizona ● Donor Network Of Arizona ● Health Current ● Health System Alliance of Arizona ● Right Care Foundation
April 24th, 2018
Cronkite News reporter Madison Stark shares how the RightCare Foundation is changing the way people think about CPR before emergency vehicles arrive.
A former Phoenix firefighter offers CPR training | Cronkite News
CPR training that uses chest compressions only is meant to prevent brain damage.
Posted by Cronkite News on Tuesday, April 24, 2018
August 31, 2017
RightCare was recently endorsed by the National Association of Emergency Medical Physicians – Arizona Chapter! Dr. Steven Maher is Chapter President and sited our “work to improve survival and neurological outcomes in the event of sudden cardiac arrest by promoting and teaching best practice Immediate Resuscitation in our community” and our “work to ensure that individual advanced directive wishes are honored” as the basis for the association’s endorsement.
RightCare is the first entity to be endorsed since their chapter began in November, 2016.


Promoting and teaching best practice Immediate Resuscitation in our community.
 January 1, 2017
January 1, 2017
The City of Phoenix has increased the out-of-hospital cardiac arrest survival rate by 5 times!
This was possible through the implementation of leading-edge pre-hospital resuscitation protocols and the establishment of a hospital network of Cardiac Arrest Centers.
Though this is great news for The City of Phoenix, we hope to continually improve the quality of emergency care to our citizens.
The Sky Harbor International Airport has demonstrated a cardiac arrest survival rate of almost 80%! This is due to the great number of BLS/AED trained personnel and great number of automated external defibrillators available at the Sky Harbor. This life-saving emergency care at Sky Harbor serves as an example of what a community can accomplish with the appropriate resources.
The RightCare Foundation advocates for this best-practice emergency care in care homes/ facilities in Arizona.
Arguably seniors are more likely to experience sudden cardiac arrest than the average visitor to Sky Harbor International Airport.
The RightCare Foundation’s goal is to dramatically increase the rate of survival of seniors that experience sudden cardiac arrest in Arizona. “We intend to influence change requiring that the same emergency care that is available at our airport be available to consumers of senior care in our community”.
Please contact us for a complimentary copy of the PowerPoint presentation by Dr. John Gallagher, Medical Director of The City of Phoenix Fire Department, detailing the great work being done in Phoenix.
 July 15, 2016
July 15, 2016
In California, an elderly woman died at a senior independent living facility after a 7-minute call between a 911 dispatcher and a nurse who refused to administer CPR which slowly stole her life away. While the company is conducting “a thorough review” of the proceedings, it was known ahead of time that CPR was “against their [company] policy.” Despite this legality, the 911 dispatcher becomes shocked and frustrated, pleading for someone – passerby or another senior citizen in the facility – to provide CPR, even offering to direct someone through it. Today show contributor, Dr. Roshini Raj reminds the public of the importance of CPR because “minutes make a difference.” Explaining that the human brain physiologically starts to die after 4 minutes due to lack of oxygen: halfway through the 911 call, the elderly woman was already dead.
Questions about the ethical and moral obligations of the nurse were discussed in the Today show clip. While it is shocking to comprehend how or why another human being would allow another person to die when they are fully qualified, this clip only scratches the surface of the inadequate systems in place in senior independent living facilities.
One important takeaway Dr. Raj made was for the public to remember that Good Samaritan Laws legally protect you if you see someone who is not breathing and try perform CPR on them – no matter the outcome. In effect, this nurse, though she could have lost her job, would have been protected by the legal system in place.
The premise, mission and lifeblood of RightCare Foundation is to help prevent tragedies like this from happening. With the proper CPR | AED training and equipment, lives can and will be changed, and minutes can turn into more years of vibrant life.
Click to see the full Today Show segment.
 December 15, 2015
December 15, 2015
The behind-the-scenes look at how Phoenix paramedics and friend, Tina Johnson, saved popular KPNX-TV Channel 12 sportscaster Bruce Cooper’s life.
When seconds counted, there is a huge team effort put forth to save the life of a heart attack victim – and the famous broadcaster – affectionately known as ‘Coop’ was no exception.
Tina Johnson, Cooper’s daughter’s realtor, began performing CPR after he fainted moving boxes. Just moments earlier he had complained about pain in his lower back. From the time paramedics arrived at the scene to him entering the hospital Cooper had coded or “flat-lined” not once, but twice.
 “I find life a lot more precious. I’m really glad that I can stay around a little while longer that I can be with my wife and daughter,” Cooper told Brad Cesmat on ‘Big Guy on Sports. “As you know there was a period not long ago that we lost our son [former Oakland Raiders linebacker Marquis Cooper, who died in a high-profile boating accident in Florida in 2009]. Just having our family together is really important.”
“I find life a lot more precious. I’m really glad that I can stay around a little while longer that I can be with my wife and daughter,” Cooper told Brad Cesmat on ‘Big Guy on Sports. “As you know there was a period not long ago that we lost our son [former Oakland Raiders linebacker Marquis Cooper, who died in a high-profile boating accident in Florida in 2009]. Just having our family together is really important.”
The station ran a special at the end of the story encouraging CPR training through the American Red Cross and even offered a 15% discount off of classes. This is another story emphasizing the importance of CPR | AED training and equipment and underscores the RightCare Mission to help save lives.
 January 1, 2014
January 1, 2014
On October 5, 2009, Terry Schoen suffered a sudden cardiac arrest at his place of business. Two of Terry’s coworkers witnessed the arrest and within seconds put
their training to use. Phoenix Fire Paramedics arrived on the scene and began advanced life support treatment. The paramedics transported Terry to a local hospital where doctors continued his care. Terry was later discharged from the hospital with no permanent damage.
Two and a half years later, Terry is enjoying life to the fullest and would like to share his story. Come talk with Terry, the Phoenix Fire crews who treated him and Dr. John Gallagher about the value of early CPR and the lives that can be saved.
Press opportunity to speak with 2-year cardiac arrest survivor
& Phoenix Fire Paramedics on the value of bystander
CPR as a vital component of the chain of survival
WHAT: Phoenix Fire Paramedics will discuss the vital role early CPR plays in the survival of sudden cardiac arrest victims
WHEN: Thursday March 29, 2012 at 10:00 AM
WHERE: Phoenix Fire station #17 — 1531 E. Missouri, Phoenix
Contact: Captain Scott Walker at 602-309-2058
Released 3/27/2012
 June 15, 2013
June 15, 2013
The words – I’ll take care of you – must have been a relief to the woman, who was failing in her later years and began falling and worrying what would become of her. Because she was old and frail and basically alone, she gave away her house to the owner of an assisted living facility.
Now the owner of that facility, Maria Barbu, has been charged with theft, fraud and forgery. Phoenix police say Barbu took Pauline Balseiro’s home, her antique furniture, her jewelry, her fur coats.
She’s also accused of forging checks on the elder lady’s accounts…
Although the perpetrator was charged with theft, fraud and forgery; This article, whose title and excerpt are featured above and that originally appeared on AZ Central, is an extremely important piece that The RightCare Foundation feels is a prime example of what continues to feed our energy and keeps our passion alive on improving the quality of senior care in our community.
 December 15, 2012
December 15, 2012
In our continuous efforts to provide the community with important information, we wanted to share a Continuous Chest Compression (CPR) video
from the University of Arizona.
RightCare supports all efforts for life saving measures and this video is a valuable resource in our ongoing efforts to assist the community.
 June 15, 2012
June 15, 2012
The recent headline, “Woman arrested for abuse of nearly 70 vulnerable adults,” explained the facts surrounding the closing of three long-term care facilities in Phoenix, but the article shows the extent of the abuse the residents had to endure.
While disturbing, the story is actually a victory for ensuring Right Care in our community and the underlying story is just as important.
Phoenix Departments Unite to Improve Care and Patients Lives
Though each city department operates under its own management, City of Phoenix Fire, Police and Neighborhood Services department personnel worked collectively to help bring the abuse to light and see that charges were filed and victims were relocated – resulting in dramatically improved conditions for 70+ assisted living care consumers.
This kind of “grass roots” first responder community involvement embodies The RightCare mission. We applaud The City of Phoenix for ensuring continuous quality improvement regarding care for its citizens.
